3 results
Meta-analysis of the variability in the individual response to pharmacological treatments for mania in bipolar disorder
- G. Anmella, M. De Prisco, V. Oliva, M. Sanabra, L. Fortea, M. Ortuño, G. Fico, A. Murru, E. Vieta, D. Hidalgo-Mazzei, A. Solanes, J. Radua
-
- Journal:
- European Psychiatry / Volume 66 / Issue S1 / March 2023
- Published online by Cambridge University Press:
- 19 July 2023, p. S84
-
- Article
-
- You have access Access
- Open access
- Export citation
-
Introduction
Many studies have investigated whether there exist predictors of good response to antimanic drugs in bipolar disorder (BD). However, these factors predict response or only indicate benign illness course.
ObjectivesTo shed some light on the topic, we tested whether the response to antimanic drugs showed any variability beyond that expected by the effects of illness course and placebo.
MethodsWe included all double-blind, placebo-controlled RCTs of oral pharmacotherapies targeting adult patients with acute bipolar mania from 1991 to 2020. The primary outcome was the variance of the improvement in manic symptoms in treated individuals compared to placebo. The effect size was the log variability ratio (logVR). We performed a random-effects meta-analysis, including assessments of heterogeneity, sensitivity/cumulative/subgroup analyses, and meta-regression.
Results42 RCTs (46 comparisons) from a total of 8,438 BD patients with acute mania (53.7% male, mean age=39.3; 5,563 treatment/2,875 control groups) were included in the analysis. Individuals in active treatment groups did not show variability in the response beyond that observed in individuals under placebo (VR=1; 95% C.I.=0.97,1.03; p-value=0.97). No heterogeneity was detected between the studies (I2=0%; tau2=0%; Q=29.21; df=45; p-value=0.97). Results were similar in the leave-one-out/cumulative/subgroup analyses. Meta-regression did not show influences by age, sample size, sex, severity of manic symptoms at baseline, or clinical features (rapid cycling, mixed or psychotic features).
ConclusionsThis meta-analysis shows no evidence of differences in the individual response to treatments. These findings suggest that the average treatment effect is a reasonable assumption for the individual BD patient with acute mania. The presented article adds evidence to the equivalent results in schizophrenia-spectrum disorders, clinical high-risk state for psychosis, and major depressive disorder, not supporting classification in responders vs. non-responders. However, these findings should be balanced with results from other fields supporting such classification.
Disclosure of InterestNone Declared
Psychological trauma as a transdiagnostic risk factor for mental disorder: an umbrella meta‐analysis
- B. M. Hogg, I. Gardoki-Souto, A. Valiente-Gómez, A. Ribeiro Rosa, L. Fortea, J. Radua, B. L. Amann, A. Moreno-Alcázar
-
- Journal:
- European Psychiatry / Volume 66 / Issue S1 / March 2023
- Published online by Cambridge University Press:
- 19 July 2023, pp. S982-S983
-
- Article
-
- You have access Access
- Open access
- Export citation
-
Introduction
This umbrella review is the frst to systematically examine psychological trauma as a transdiagnostic risk factor across psychiatric conditions.
ObjectivesThis review aimed to be the frst to evaluate whether psychological trauma fulflilled criteria as a transdiagnostic risk factor cutting across various diagnostic categories and spectra. Transdiagnosticity will be assessed against the framework of the TRANSD criteria (Fusar-Poli, World Psychiatry 2019; 18 361-362). The paper additionally aimed to analyse the association of psychopathology with specifc trauma type.
MethodsWe searched Pubmed, Scopus, and PsycNET databases from inception until 01/05/2021 for systematic reviews/meta-analyses evaluating the association between psychological trauma and at least one diagnosed mental disorder. We re-calculated the odds ratio (OR), then classifed the association as convincing, highly suggestive, suggestive, or weak, based on the number of cases and controls with and without psychological trauma, random-efects p value, the 95% conf- dence interval of the largest study, heterogeneity between studies, 95% prediction interval, small-study efect, and excess significance bias. Additional outcomes were the association between specifc trauma types and specific mental disorders, and a sensitivity analysis for childhood trauma. Transdiagnosticity was assessed using TRANSD criteria. The review was pre-registered in Prospero CRD42020157308 and followed PRISMA/MOOSE guidelines.
ResultsFourteen reviews met inclusion criteria, comprising 16,277 cases and 77,586 controls. Psychological trauma met TRANSD criteria as a transdiagnostic factor across diferent diagnostic criteria and spectra. There was highly suggestive evidence of an association between psychological trauma at any time-point and any mental disorder (OR=2.92) and between childhood trauma and any mental disorder
(OR=2.90). Regarding specifc trauma types, convincing evidence linked physical abuse (OR=2.36) and highly suggestive evidence linked sexual abuse (OR=3.47) with a range of mental disorders, and convincing evidence linked emotional abuse to anxiety disorders (OR=3.05); there were no data for emotional abuse with other disorders.
Image:
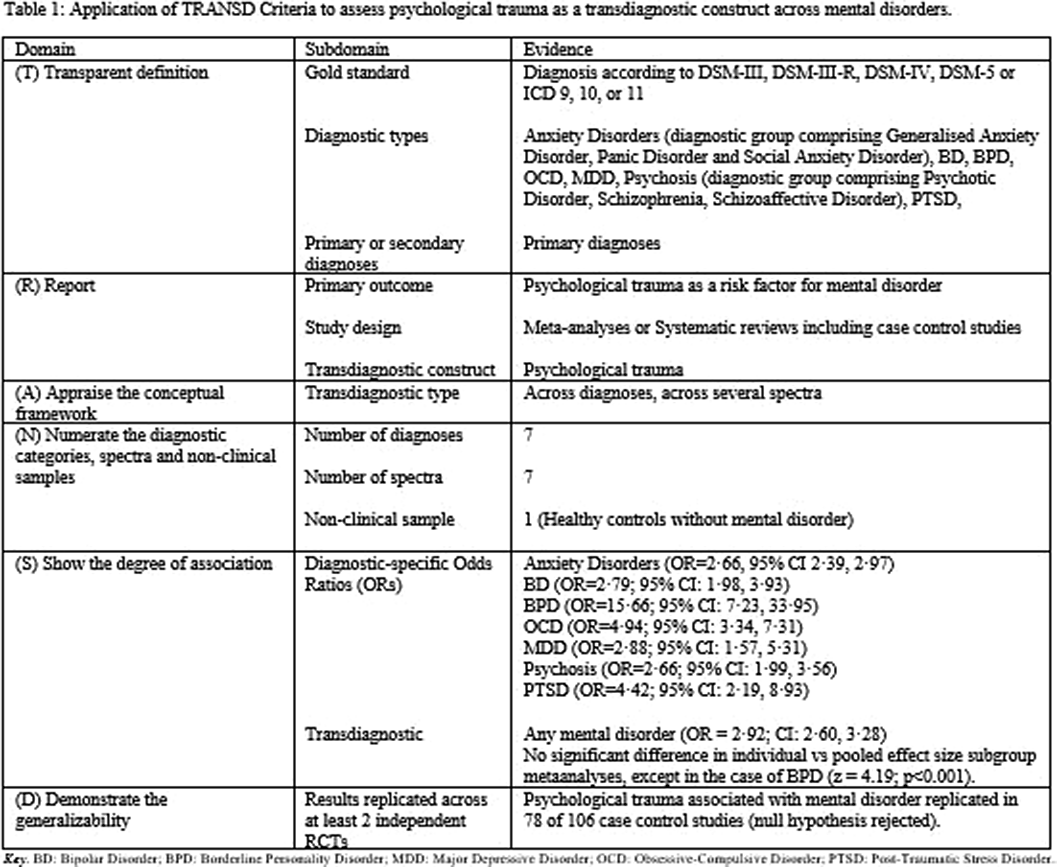
Image 2:
 Conclusions
ConclusionsThese fndings highlight the importance of preventing early traumatic events and providing trauma-informed care in early intervention and psychiatric services.
Disclosure of InterestNone Declared
Suicide attempt in alcohol use disorder and Wernicke encephalopathy: A case report
- L. Espinosa, A. Fortea, G. Oriolo, M. Balcells, C. Oliveras
-
- Journal:
- European Psychiatry / Volume 33 / Issue S1 / March 2016
- Published online by Cambridge University Press:
- 23 March 2020, p. S599
-
- Article
-
- You have access Access
- Export citation
-
Background
The relation between alcohol dependence and suicidal behavior is well known and alcohol consumption is a risk factor to take in consideration in order to prevent suicidal attempts. Wernicke encephalopathy (WE) is a common acute neurological disorder caused by thiamine deficiency frequently associated with alcohol use disorder and often infra-diagnosed. Just few cases are reported about the possible correlation between suicidal behaviour and Wernicke encephalopathy.
ObjectiveTo describe the possible association between suicidal attempts and Wernicke encephalopathy.
MethodsWe report the case of a 57 year old man, with past diagnosis of disthymia and amphetamine abuse disorder, and a history of bariatric surgery, who was hospitalized in the intensive care unit (ICU) of hospital clinic for a suicidal attempt by mean of metro railway precipitation. He presented two episodes of psychomotor agitation in the context of an abstinence syndrome that reverted with midazolam continuous perfusion and clonazepam 8 mg per day. Consequently to medical improvement, he was moved to Psychiatry Unit of Addictive Behavior and finally diagnosed with alcohol use disorder.
ResultsIn the physical exam, bilateral nystagmus and cerebellar ataxia were observed. Signs of malnutrition were detected in the blood analysis. In a brain magnetic resonance image, volume deficits in the mammillary bodies, thalamus, cortex and corpus callosum, as well as peri-aqueductal altered signal were observed, all signs compatible with Wernicke encephalopathy diagnoses.
ConclusionsWernicke encephalopathy is a frequent concomitant condition in patients with alcohol use disorder. The consequent cognitive decline could represent an independent added risk factor for suicidal behavior.
Disclosure of interestThe authors have not supplied their declaration of competing interest.





